Back to Resource Center / Insights / Posted on 03-03-2026
How often should PBM audits be conducted?
- Ethica recommends auditing PBM contracts and financial terms annually, but at a minimum, once per contract term, which is typically 3 years.
Warning signs or quiet indicators
 No previous audit – With enhanced scrutiny on PBMs and the growing focus on PBM reform, self‑funded plan sponsors who have never conducted an audit should make it a priority.
No previous audit – With enhanced scrutiny on PBMs and the growing focus on PBM reform, self‑funded plan sponsors who have never conducted an audit should make it a priority.
 Performance trending off track – At Ethica, we track PBM contract performance in our quarterly dashboards and assess when a PBM may miss its contract guarantees. This is a prime indicator that an audit is needed.
Performance trending off track – At Ethica, we track PBM contract performance in our quarterly dashboards and assess when a PBM may miss its contract guarantees. This is a prime indicator that an audit is needed.
 Unexpected rebates or savings variability – Unexplained or significant differences between expected and actual results can indicate issues.
Unexpected rebates or savings variability – Unexplained or significant differences between expected and actual results can indicate issues.
 PBM transitions – Whether working with a new PBM or undergoing operational changes with the existing one, transitions are a strong reason to initiate a review.
PBM transitions – Whether working with a new PBM or undergoing operational changes with the existing one, transitions are a strong reason to initiate a review.
Why details make a difference
- High-risk areas for PBM discrepancies
Rx pricing is incredibly complex. There are multiple pricing types, distribution channels, rebates and administrative fees, PMPM guarantees, and shared-savings arrangements. We see discrepancies across all of these components.
- The cost of small inaccuracies over time
A plan design and drug coverage audit is a clear example of how small inaccuracies can compound. During an audit, we often find that drug exclusions are not coded correctly, resulting in the Plan covering medications that are clearly noted as excluded in the SPD. Without regular audits, these plan coverage errors can continue indefinitely without the Plan’s knowledge.
The risks of not auditing
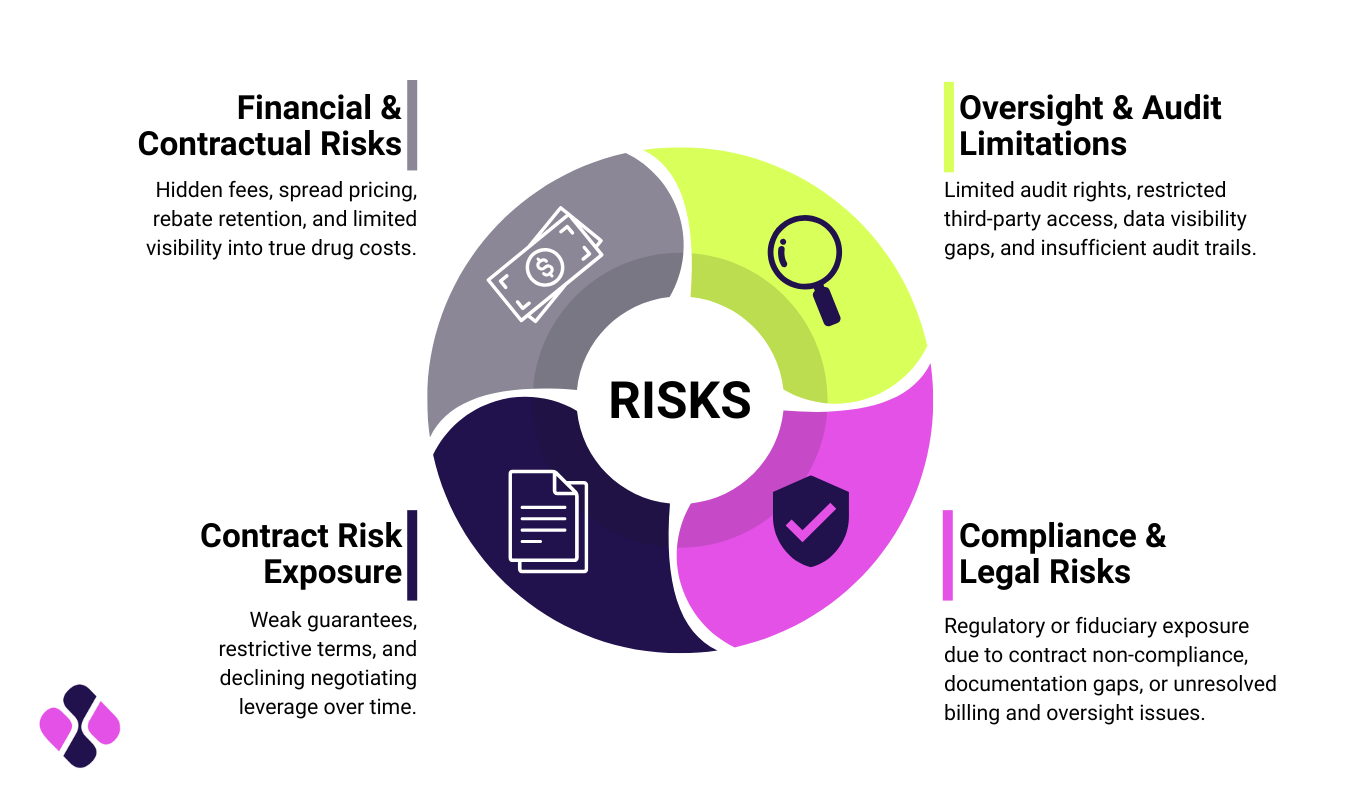
Note:
Organizations should engage independent experts to review PBM contracts for transparency requirements, pricing guarantees, audit rights, and performance metrics before signing. This verification process can save significant costs and protect against these various risks.
Why PBM audits matter
- Balancing savings & patient care
PBM audits support both cost control and patient access to medications by identifying recoveries from shortfalls on contract guarantees and uncovering instances where the PBM inappropriately covers excluded drugs.
- How transparency supports better decision-making
By improving transparency, audits can serve not only as governance and due diligence on a large healthcare cost item but support positive changes across vendor selection, negotiations, plan coverage and performance guarantees.
Key Takeaways
Audits shouldn’t be reactive — they should be a standard component of PBM oversight.
Ethica Pharmacy Advisors provides independent auditing expertise to help organizations strengthen transparency, validate performance, and ensure their pharmacy benefits operate as intended. Reach out to Ethica to learn how a comprehensive audit can support your organization’s goals and guide your PBM strategy forward.
Back to Insight Center
Let’s make it make sense.
Pharmacy benefits clarity begins with our market analysis where we reveal data-driven insights and identify opportunities to help you make more informed decisions.
